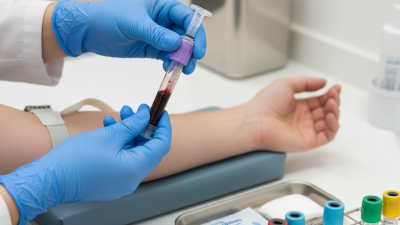
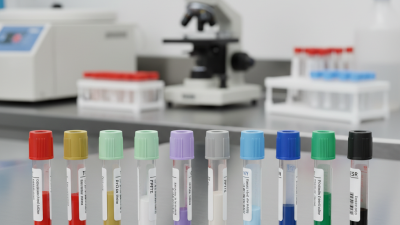
When working in a clinical setting, the proper use of a vacutainer is crucial. Vacutainers are essential for collecting and transporting blood samples safely. However, improper usage can lead to contamination and inaccurate results. This article provides ten essential tips to enhance the effectiveness of vacutainers in your lab work.
Understanding the correct technique is vital. For instance, the angle of insertion can greatly affect blood flow into the vacutainer. Additionally, not all vacutainers are the same; selecting the right type for specific tests is key. Many novice users overlook the expiration dates of these tubes, leading to compromised samples. Thoughtful attention to detail makes a significant difference in outcomes.
Despite the convenience of vacutainers, challenges persist. Users may face difficulties in blood drawing techniques or experience issues like hemolysis. Reflecting on these experiences is important for improvement. By following these tips, healthcare professionals can enhance their competence and ensure they use vacutainers effectively for reliable testing.
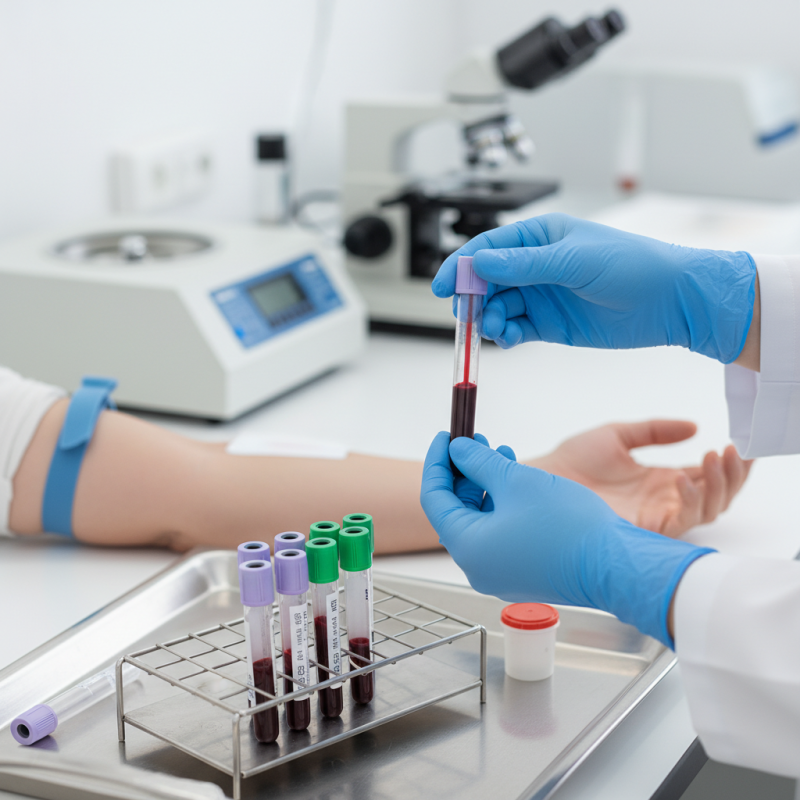
Understanding Vacutainers and their types is crucial for successful blood sampling.
Vacutainers are essential tools in laboratories and medical settings. They come in various colors, each indicating different additives for specific tests.
The most common types include serum tubes, EDTA tubes, and sodium citrate tubes.
Each type serves a distinct purpose, affecting the sample quality and test results.
Tip:
Always select the correct tube type. Using the wrong tube may lead to erroneous results. For instance, serum tubes are often used for biochemical tests, while EDTA tubes are ideal for hematological assessments.
The choice impacts the analysis significantly. A study by the Clinical Laboratory Standards Institute showed that improper tube selection can lead to up to 30% of the tests being inconclusive.
Additionally, proper handling of Vacutainers is vital. Ensure that the tubes are filled to the correct volume. Underfilling or overfilling can cause issues during sample analysis.
Keep in mind, blood samples should be processed within the recommended time frame. Delayed processing can result in cellular changes, affecting test results.
Tip:
Always check expiration dates on tubes. Expired tubes may compromise sample integrity. Understanding the science behind Vacutainers is key.
Knowledge of additives can enhance accuracy and reliability in patient diagnostics, leading to better healthcare outcomes.
Selecting the right vacutainer is crucial for accurate test results. Different tests require specific types of vacutainers to work effectively. For instance, blood cultures often need special bottles to minimize contamination. Other tests might need additives like anticoagulants or serum separators. Knowing these requirements can save time and prevent errors.
Each vacutainer color represents a different additive or purpose. For example, a red-top vacutainer is typically used for serum tests. On the other hand, a lavender-top tube is meant for blood counts. This color-coding system streamlines the selection process but requires careful attention. Not knowing the differences may lead to mix-ups.
Mistakes can happen, even in a routine process. It’s essential to double-check the requirements for each test. If unsure, consult your lab's guidelines. Investing time in understanding vacutainer types helps ensure the accuracy of tests. This knowledge ultimately enhances patient care, making it a vital aspect of any laboratory process.
When collecting blood samples, proper techniques are essential for accurate results. Always ensure that the vacutainers are undamaged and clean. Use a tourniquet to fill the veins but apply it gently to avoid discomfort. Palpate the vein to locate the best puncture site. A common mistake is to choose a difficult vein, causing more pain and anxiety for patients.
Maintain a steady hand when inserting the needle. A slight angle of 15 to 30 degrees works best for access. Don't rush; sudden movements can complicate the process. If blood does not flow immediately, gently reposition the needle without pulling it out. This emphasizes the importance of patience and observation.
Once blood flows into the vacutainer, release the tourniquet. Fill the tube to the required level but avoid overfilling or underfilling. Discard any samples that do not meet the standards. Lastly, always label the samples accurately and promptly. This step is critical to avoid mix-ups in the lab. Keeping these techniques in mind will enhance the quality of blood collection and promote patient safety.

Labeling and storing samples accurately are critical for effective use of Vacutainers. Proper labeling ensures that each sample is identifiable and traceable. Research shows that mislabeling can lead to diagnostic errors in up to 20% of cases. Always include patient name, date of collection, and type of sample. Use waterproof and smudge-proof markers to enhance label durability.
When it comes to storage, temperature is vital. Samples should be stored at appropriate temperatures to maintain their integrity. Studies indicate that samples stored above recommended conditions can degrade, compromising test results. Ensure that your storage facility is regularly monitored and calibrated.
Here are a couple of tips for effective practices: Clean each Vacutainer before use to prevent contamination. Also, a mix of proper storage techniques will maintain sample quality. Avoid overcrowding your storage area, as it might lead to accidents. Frequent audits of storage conditions can reveal areas for improvement.
When using vacutainers, common mistakes can undermine their effectiveness. One frequent error is improper handling. Tightly gripping the vacutainer can cause premature clotting. Instead, hold it gently to keep the blood flow smooth. Another mistake is not checking the expiration date. Using expired tubes can lead to inaccurate test results, impacting patient care.
Also, improper mixing of additives poses a risk. Some users forget to gently invert the tube after collection. This step ensures that anticoagulants and additives mix well with the blood sample. Skipping this can compromise test integrity. Additionally, failing to label the tubes immediately can lead to misidentification. A clearly labeled tube helps avoid confusion in the lab.
Finally, don't rush through the collection process. A hurried approach can lead to hemolysis, affecting results. Take your time to ensure each step is followed correctly. Reflecting on these details can improve accuracy in lab results and ultimately benefit patient outcomes.
| Tip No. | Tip | Common Mistake | Solution |
|---|---|---|---|
| 1 | Choose the right Vacutainer | Using incorrect tube type | Consult test requirements before selection |
| 2 | Check expiration dates | Using expired tubes | Regularly inspect supply inventory |
| 3 | Follow proper order of draw | Incorrect order leading to contamination | Use color-coded guides for reference |
| 4 | Use correct filling technique | Underfilling or overfilling tubes | Refer to manufacturer guidelines |
| 5 | Invert tubes gently after collection | Neglecting inversion | Follow recommended inversion times |
| 6 | Avoid hemolysis | Filling tubes too aggressively | Use gentle technique for blood draw |
| 7 | Label tubes immediately | Delayed labeling causing mix-ups | Label at the point of collection |
| 8 | Store tubes properly | Improper storage conditions | Follow storage recommendations |
| 9 | Avoid contamination | Touching the inside of the tube | Use sterile techniques |
| 10 | Transport samples promptly | Delays in sample transport | Implement a transport schedule |